PLEASE NOTE: THIS blog is a reprint of an article that appeared on Huffington Post.
How can we measure the resiliency of the Haitian people who are the poorest in the western hemisphere with 55% living below the extreme poverty line of $1 a day? On a good day in Haiti, nearly half the population doesn’t know when or where the next meal will come; in good times, 47% don’t have any access to the most basic health care; 45% of the population doesn’t have clean water and 80% are without basic sanitation. People fear going to the nation’s main hospital, which we have worked to bring to life over the last week, because at its best, it provided inadequate care in facilities with marginal electricity and water, and received no funding. When we arrived there, we found no basic medical supplies to restock the meager supplies we could fit into our bags and our small plane.
How can we measure the resiliency and capacity to endure of these people who have endured for 200 years? Perhaps it is in the strength of the 85-year-old woman found yesterday in the rubble 10 days after the quake still breathing, with a pulse and blood pressure and who after some intravenous fluids, started producing urine again. Or the little boy who a day after being found in the rubble after a week was running around our medical camp hugging the nurses and doctors who brought him back from near death? Or the 13-year-old who ran to the top of the 3-story building as it collapsed under her, riding it down to the ground suffering “only” a massive laceration to her thigh that her mother attempted to stitch without anesthesia with a needle and thread. There is barely a whimper from the hospital campus where we reduced fractures with only a little pain medication and where gaping, infected and necrotic wounds are re-bandaged daily without sedation. There is only the occasional wailing from a broken heart.
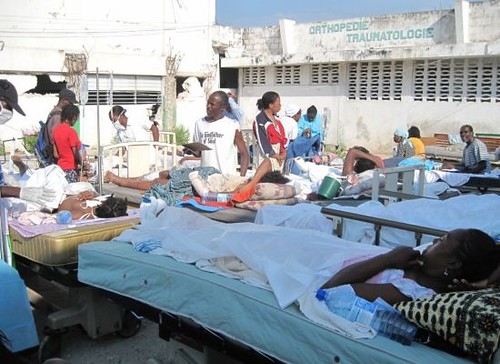
Yesterday was the first day the coordination and supplies came together on the hospital campus — with nine hospital and 3-4 NGO operating rooms working 24 hours a day now, with X-ray and ultrasound and proper surgical instruments and supplies, and medical personnel, with food, water, and tents to house the patients who crawled with broken pelvises and hopped with the newly amputated stumps dangling from the hospital wards to the open air with each shake of the ground. Finally after days of transporting patients in and out of buildings, after the U.S. Army Corp of Engineers repeated inspections, it was clear that patients were more afraid of being inside than outside. But it is very difficult to run surgical intensive care units in the open air or sweltering tents without electricity or water. And patients die.
As the immediate surgical needs are slowly addressed, the psychological needs explode magnified by each minor aftershock.
But what we see inside the walls of the hospital, which has concentrated resources, NGOs, food, water, supplies, people, however inadequate they may be, however limited our abilities to care for patients, however strained our ability to track medical records, to know which patient had which treatment and when, however great our need for better communication and coordination, the General Hospital is the most well-organized run health care facility in Port-au-Prince right now. Compared to the needs and demands of those outside its walls, those in tent cities, or lying in the streets who bathe, eat, drink and defecate all in the same few square feet, and are at risk of tetanus, or diseases of overcrowding such as meningitis, diarrhea, typhoid, hepatitis, measles, diphtheria, whooping cough or tuberculosis, or the millions displaced or whose lives are upside down, General Hospital is the now the Mayo Clinic of Haiti. But the load of new surgical cases at the General is diminishing though we still have to clean and eventually close the hundreds of stumps and wounds we have treated already. Local doctors at the hospital express concern that we have seen all the patients to be seen, and are worried about sending patients off the USS Comfort or other mobile hospitals coming in. But they have not accounted for the second wave.
The Second Wave: The Forgotten Thousands
There will be a second wave, there must be a second wave and it must come now or it will be too late. There have already been too many tragic deaths in the immediate aftermath of the quake, but now there will be thousands of unnecessary, preventable deaths from the consequences of the lack of medical care from infection, gangrene and tetanus. There is simply a lack of infrastructure.
There are few ambulances or EMTs in Haiti and I have only seen one or two in the streets. There is barely fuel, with prices shooting up to $800 USD a gallon at one point, in a country where a good wage is $100 a month, where 900 gallons of diesel to run the hospital generators were stolen from the back gate before the military arrived. The initial effort by FEMA providing $36 million for search and rescue was critical to save lives. Now 11 days later, there is a need for emergency medical response teams to find and scoop and transport the thousands remaining strewn about the city. According the USAID daily report, there was only $50,000 spent on emergency medical response to date.
It is dire, even the dogs are hungry. They chewed to the bone a leg of a dead man sticking out of the rubble.
Last night flying back on a C 17 Air Force transport, I spoke to Miami firefighters who surveyed the city and reported that they saw no search and rescue teams any longer, only two ambulances and two pieces of heavy equipment. But when they walked through tent cities and streets and they found hundreds of patients who needed to get to a hospital for emergency care but had no way of getting there, now way of being identified and were not aware of available resources or hospitals. Cell phones work only occasionally, there is a breakdown of communication infrastructure. One hospital they visited remained nearly empty with doctors roaming the streets looking for patients.
The immediate burden on the hospital campus has been addressed, but there are thousands tucked in corners of alleyways, under tarps, in tent cities all over Port-au-Prince and surrounding areas that have not had medical care, still with open fractures, gaping wounds, crush injuries that are stuck without knowledge of where medical facilities are, or any way to get transported and afraid to leave their meager belongings unattended on the sidewalk or by their tent or tarp.
Yesterday I heard about Jackmel, a nearby city, where 30 critical victims needing amputations or emergency surgical care have been trapped by damaged roads and isolated since the quake with no food, water, and medical care waiting for 11 days to get evacuated. I worked yesterday with General Keen to find a way to get those patients mobilized. And those are only the ones I have heard about, how many more are there? There are thousands more unattended who now are at risk of unnecessary death from gangrene and infection and tetanus, thousands more who could have their limbs or lives saved if we can get to them in time.
Coordination between the military, government and volunteer resources is happening but slowly. A clear plan needs to be developed immediately to deploy volunteer EMT’s, translators and security and transport with a map of all existing medical resources, functioning communication to immediately find and bring those patients to medical care. Fliers, radio announcements, trucks with loudspeakers can be deployed through the city to flush out the patients needing care.
Third Wave: Discharge Planning, PTSD, and Rehab
Then there is the third wave. Once we treat and stabilize the patients, there is nowhere for them to go. Their homes are piles dust and rust, their families gone. Who can tend to them, feed them, change their bandages? Where can they live, who will transport them back to the doctor or hospital for follow up visits? We can’t send them back to the street. I spent two hours yesterday with Navy doctors Richard Sharpe and Larry Ronan from the USS Comfort to find an open space to put post-operative patients. We are at capacity. And all the hospitals in the country are full.
Soon, very soon, there is the need for rehabilitation, helping the thousands with lost or broken limbs get back on their feet or foot again. There are no physical therapists, no facilities, and no place for them to go for care. As the immediate surgical needs are slowly addressed, the psychological needs explode magnified by each minor aftershock. There are no psychologists here. The Center for Mind Body Medicine that has worked on PTSD in Kosovo, Gaza and New Orleans is mobilizing a team of 500 to go to Haiti over the next months coordinated with Partners in Health. But more will be needed.
Coordinated planning is needed to provide food, water, sanitation, dressing changes and skilled nursing care, and it is needed now in large temporary tents properly staffed by local Haitians providing jobs and care, closing the ecosystem of health and recovery. Plans are being developed to move people out of Port-au-Prince to begin to rebuild and restore the city infrastructure, utilities, and housing. The local Haitian medical community has to be supported and restored to care for the traumatized for the long term. The partnership model of Partners in Health training and employing local community health workers providing jobs and bolstering the Haitian economy, which they have done now in a dozen locations in Haiti, employing 5000 Haitians is essential if we are to avoid a hit and run NGO disaster relief that will only leave another disaster. Last night we scrambled to find a way to take over the Israeli field hospital and care for the 150 patients still there when they leave on Wednesday.
The Silver Lining: Empowering the Haitian People
They have done their job, but rebuilding Haiti will not take a week or a month or a year, but decades of sustained and coordinated effort needed when the disaster relief is over. Haitians must be empowered to take back their country and create what they have always deserved. They were the first liberated from slavery in the early 1800s but yet to be lifted from extreme poverty.
Aside from my day job, I am a volunteer for Partners In Health (PIH), which has been working on the ground in Haiti for over 20 years. The organization works to bring modern medical care to poor communities in nine countries around the world. The work of PIH has three goals: to care for patients, to alleviate the root causes of disease in their communities, and to share lessons learned around the world. Based in Boston, PIH employs more than 11,000 people worldwide, including doctors, nurses, and community health workers. The vast majority of PIH staff is local nationals based in the communities they serve. They can partner with other organizations and the local Haitian government and communities to effectively and for the long-term support the emergence of the enduring, resilient and openhearted people from two centuries of darkness. Donate at http://www.pih.org.
Please share your thoughts by leaving a comment below.
To your good health,
Mark Hyman, MD
To see more of Dr. Hyman’s photos from Haiti go to:
http://www.flickr.com/photos/drhyman/sets/72157623158256281/
Beware: Some of the images are graphic.